Referral criteria
Babies, children and young people with life-limiting conditions requiring palliative and end-of-life care.
Families of babies, children and young people who have died requiring specialist bereavement care.
Palliative and end-of-life care criteria
- Introduction
- Age criteria
- Geography
Introduction
Babies, children and young people with a life-limiting or life-threatening condition who are unlikely to reach their 18th birthday.
To be accepted, babies, children and young people must meet all the criteria below.
- Age criteria
- Geographic criteria
- Life-limiting criteria, which can be either:
- General medical criteria if diagnosis is unknown
- Specific medical criteria which falls into one of the categories below.
Information about age and geographic criteria can be found on the tabs next to this. General and specific medical criteria each have their own sections below.
Age criteria
- Aged from pre-birth to 18th birthday.
(If a child is referred before birth with a life-limiting or life-threatening condition then if they are “stillborn” the family would be eligible for bereavement care).
However post-death referrals cannot be made for families of babies who are “stillborn”. - Young people aged 18–21 years and already receiving a service from SSCH can continue until the day before their 21st birthday unless:
- successfully transitioned to another service
- discharged from the service
- New referrals for young people aged over 16 years will be assessed sensitively according to life expectancy and needs.
Every effort will be made to investigate ongoing support options after 19 years if required.
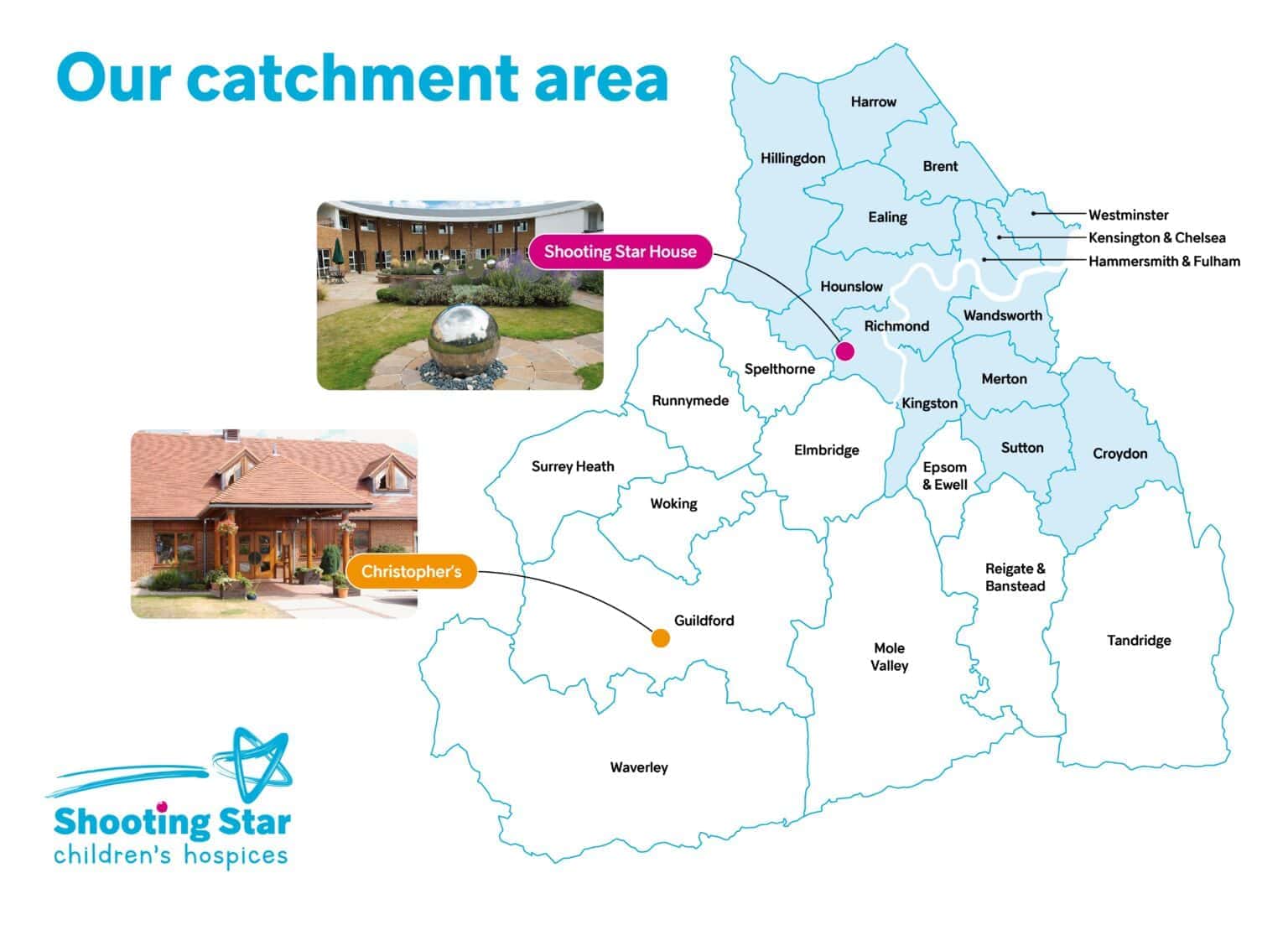
Geography
- Families must reside or attend a GP practice within the County of Surrey or in one of the 14 London Boroughs: Hammersmith and Fulham, Kensington and Chelsea, Wandsworth, Westminster, Brent, Croydon, Ealing, Harrow, Hillingdon, Hounslow, Kingston upon Thames, Merton, Richmond upon Thames, Sutton.
- Exceptional circumstances:
If a child does not have access to a children’s hospice service and they are outside our catchment area, SSCH will review and consider acceptance on a case‑by‑case basis.
General medical criteria
There are a wide range of life-limiting and life-threatening conditions affecting children and young people.
Some children and young people can be readily accepted as meeting hospice criteria since their diagnosis informs that their condition is not expected to reach adulthood. However, with medical advances, prognostication can shift. Complex medical conditions often remain uncertain when considering prognosis.
We consider two general questions:
Does the child or young person have a life-limiting condition where they most likely will die prior to their 18th birthday?
(Use specific medical criteria to provide evidence; must fit one of the four TfSL categories.)
“Would you be surprised that this baby/child/young person died before their 18th birthday?”
TfSL Categories
Category 1
Life-threatening conditions for which curative treatment may be feasible but can fail.
Access to palliative care services may be necessary when treatment fails or during an acute crisis.
Category 2
Conditions where premature death is inevitable.
There may be long periods of intensive treatment aimed at prolonging life and allowing normal activities.
Category 3
Progressive conditions without curative treatment options
Treatment is exclusively palliative and may commonly extend over many years.
Category 4
Irreversible but non-progressive conditions causing severe disability, leading to susceptibility to health
Children can have complex health care needs, a high risk of an unpredictable life-threatening event or episode, health complications and an increased likelihood of premature death.
Specific criteria: children and young people
- Severe cardiac conditions that may not be amenable to surgery, or only with severe morbidity.
- Non curative or unstable cardiac condition awaiting surgery
- Severe Cardiomyopathy (maybe waiting for transplantation or severe impact on daily living)
- Stage 3 with additional cardiac symptoms
- stage 4 and 5 as confirmed by their neurologist.
-
- Severe gut failure including those which may require TPN
- Uncontrolled reflux causing recurrent aspiration with hospitalisation
- Weight loss or static weight despite optimised feed regime
- Pain and distress associated with feeding and progressive feed reduction
- GI Dystonia
- Severe chromosomal abnormality, e.g. Trisomy 13 and 18 (including mosaicism), triploidy.
- Post-natal exome sequencing indicates potential to lead to death in early childhood.
- Multiple severe abnormalities (may or may not be treatable) in the absence of a clear diagnosis
- Multisystem failure requiring intensive care support
- Infants (0-24months) with acquired brain injury (longer-term prognosis is not always clear for younger
children, accepted without additional neuro-disability criteria)
Additional Criteria (for those >24months old):
Have 2 of the following:
- Vulnerable unsupported airway, e.g. Stridor, apnoea, requiring airway repositioning
- Recurrent aspiration events
- Severe scoliosis that compromises respiratory function
- Repeated prolonged and severe chest infections requiring intervention/antibiotics
- Ongoing need for oxygen therapy or ventilatory support
- Frequent, unplanned hospital admissions
- Escalating medical interventions
- GI Dystonia
- Severe dystonia requiring specialist palliative care support
- Severe pain or other complex symptoms requiring specialist palliative care input
- Central shut down including apnoea, bradycardia, vasomotor changes, period of unresponsiveness or altered level of consciousness
- Any child who is receiving specialist palliative care input
- Any child who has relapsed/refractory disease including a bone marrow/stem cell transplant or CAR-T therapy.
- Any child with a cancer that is known not to be curable at diagnosis
- Confirmed, or highly suspected (by neurologist) progressive neuromuscular or neurological condition, where death is likely prior to 18th birthday due to diagnosis, or they meet neuro-disability additional criteria (see Neuro-disability section)
Any child on Oxygen:
- If they fall into another supporting category
- If they are not for escalation to Long term ventilation
Any child on non-invasive ventilation in the community requires additional criteria:
- Meets criteria with another diagnosis or
- additional ventilation support considered a destination therapy e.g. due to primary respiratory failure or progressive central respiratory failure. This excludes conditions including primary obstructive sleep apnoea unrelated to neurodisability.
- Increasing or reaching limits of oxygen or non-invasive ventilation requirements or
- Advance care plan states not for CPR and/or escalation to PICU or
- Has recurrent hospital admissions for airway clearance or lower respiratory tract infections
Any child with a Tracheostomy requires additional criteria:
- Meets criteria with another diagnosis or
- Requires ventilation support and/or regular oxygen therapy or
- Has recurrent hospital admissions for lower respiratory tract infections
- Complex and/or poorly controlled seizures defined by the need for 3 or more anticonvulsants, can be less in situations where multiple medications trialled yet deemed unsuccessful, or need for rescue medication at least every 2 weeks.
- A known seizure disorder that is considered life limiting
- A seizure disorder that is considered refractory to medication, as described by a neurologist
- Are seizures poorly controlled requiring frequent hospital admissions or admissions to intensive care
- Epilepsy disorder considered to be progressive in nature by a paediatric neurologist despite no formal diagnosis
Organ failure awaiting transplant
- Skin: Severe forms of Epidermolysis bullosa
- Skeletal: Severe skeletal dysplasia (including some osteogenesis imperfecta and Arthrogryposis.
Perinatal referral criteria
Diagnostic approach
Babies may be diagnosed before or after birth with a condition that is certainly or potentially life-limiting. The British Association of Perinatal Medicine lists these conditions, which can be used to inform perinatal-specific criteria. (see below)
Multidisciplinary team concern
Babies may be at risk of dying even if they do not have a specific diagnosis of a life-limiting condition. Members of the multidisciplinary team and parents should be encouraged to share their concerns. Consideration of palliative care does not require uniform agreement by the treating team and parents. Disagreement often indicates an uncertain prognosis and potential life limiting condition.
Surprise question
“Would it be a surprise if this baby died (in the short or longer term)?”
Perinatal-specific conditions (adapted from BAPM 2024)
- Severe lung or airway abnormality (e.g. Alveolar capillary dysplasia, laryngeal or tracheal atresia).
- Newborns where there is a question about providing tracheostomy for long-term ventilation.
- Severe congenital diaphragmatic hernia.
- Severe congenital cardiac conditions, may not be amenable to surgery, or with severe morbidity
- Severe fetal cardiomyopathy.
- Babies with short gut following bowel resection or long-term dependence on parenteral nutrition.
- Newborn infants with organ failure requiring escalation to extra-corporeal membrane oxygenation or dialysis or solid organ transplantation
- Severe congenital skin disorder e.g. Epidermolysis bullosa, Harlequin fetus.
- Severe hydrops fetalis.
- Multiple severe congenital abnormalities (may/not be treatable) in the absence of a clear diagnosis
- Newborn infants with brain injury and high risk of severe disability, e.g. infants with severe (III) hypoxic-ischaemic encephalopathy
- Neonatal or fetal onset neuromuscular disorder, e.g. myotonic dystrophy, myopathy,SMA
- Severe brain abnormality e.g. Anencephaly, Craniorachischisis, Hydranencephaly, Holoprosencephaly, Lissencephaly.
- Vein of Galen malformation.
- Very severe intra-uterine growth restriction
- Prolonged preterm rupture of membranes from early gestation with oligo or anhydramnios
- Where early screening detects possible life limiting condition a referral can be made before 20 weeks but will be held with referral only being accepted after 20 weeks.
- High risk or extremely high-risk preterm delivery ie from 22+0 weeks gestation
- Extremely preterm infants with severe complications, e.g. severe necrotising enterocolitis, intraventricular haemorrhage, cystic periventricular leukomalacia, severe chronic lung disease.
- Bilateral Renal agenesis
- Other severe renal system disorder, e.g. severe multicystic dysplastic kidneys, oligohydramnios, bladder agenesis
- Severe skeletal dysplasia (including osteogenesis imperfecta)
- Arthrogryposis with confirmed severe neuromuscular disorder
Any other criteria that meets the MDT concern and Surprise Question criteria
Specialist bereavement care criteria
Families known to the hospice can continue to receive bereavement care when their child dies. Families not known to the hospice can be referred following the death of their child.
For new bereavement referrals to be accepted (where a child was not previously accepted to the hospice), the criteria below must be met:
Age
The age criteria is 0-18 years: including families of a baby who was born alive at 22 + 0 weeks gestation or older, or a child or young person who died before their 18th birthday.
Geography
The geography criteria: family live (or attend a GP practice) within the hospice geographical catchment.
Time
The child’s death occurred within the last 18 months.
Exclusions
At this point in time, we cannot accept referrals for families whose child died by suicide or homicide, or other circumstances where an arrest has been made. Due to the individual nature of child death we reserve the right to decline any referral if we feel we do not have the resources to support the bereaved family at the time of referral.